Celebrity
Allergy news: Allergy sufferer Dr Rhiannon Grant is researching allergy disease to find a cure | Exclusive interview
Dr. Rhiannon Grant’s earliest memories are about living with allergies.
Grant, 28, was a child growing up in the NSW city of Wollongong allergies had an impact on her life for the first time.
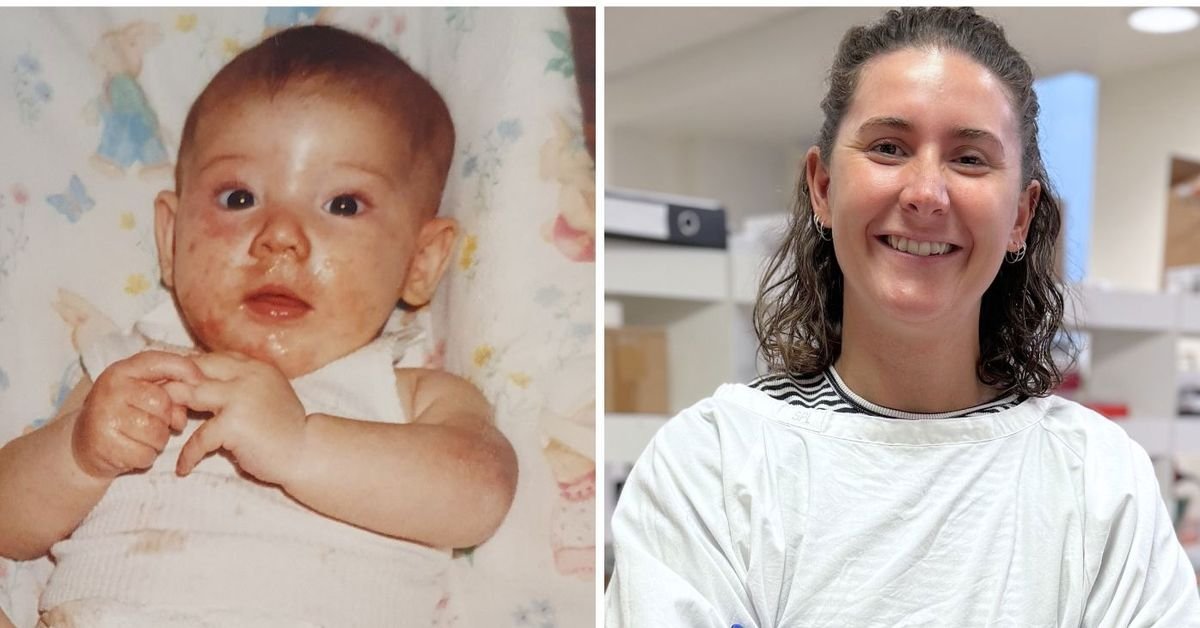
“It bothered me from the time I was a few months old eczema,” she told nine.com.au.
Watch the video above.
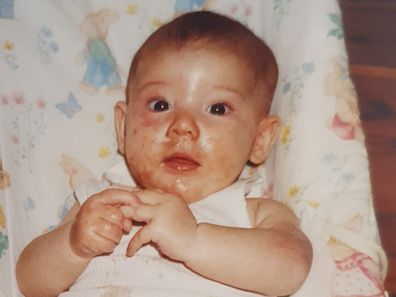
“It was on my face and most of my body as well. I grew up having to sleep every night with wet cloths and bandages all over my body and socks on my hands so I couldn’t scratch [myself] during the night.”
Simple things that other kids take for granted, like swimming lessons or sleepovers, were difficult.
“I have a memory of a sleepover in elementary school. People were making fun of each other and putting toothpaste on their faces while they were sleeping, and someone did that to my face and I got quite rash and irritated,” Grant said.
As she grew older, her primary school and teenage years were marked by recurring staph infections, caused by germs that invaded her damaged skin.
READ MORE: How Sydney dancer became the next Channing Tatum
READ MORE: Teen was told to lose weight before being diagnosed with the disease
READ MORE: Royal spotted at a society wedding after lying low

At one point, doctors gave her antibiotics for three years to prevent further infections.
As Grant got older, she learned how to take better care of her skin by moisturizing regularly, applying her steroid creams, and avoiding triggers.
But eczema wasn’t the only allergic disease that affected her life. She also suffered from asthma and food allergies – something she shared with two of her three sisters, as well as her father, aunt and uncle.
By the time she was one, Grant was diagnosed with a food allergy to nuts, eggs, dairy products, peas and potatoes, although this was later narrowed down to nuts, eggs and dairy products.
Despite the potentially life-threatening nature of her food allergies, she doesn’t remember it being made into a big deal until she started school.
“It wasn’t something I had clear memories of until I couldn’t eat cake in primary school, and realized I had to carry an EpiPen, and started to realize the impact this would have on my life,” she said.
Since allergies play such a big role in the lives of Grant and her family members, it made sense that she would one day make a career out of it.
“I was always interested in science from an early age,” she says.
“At Christmas and family gatherings we always talked about allergies and why people get allergies.
“Because so many of my family members have allergies and have been in and out of specialty appointments throughout my life, it was always a point of curiosity.”

She realized that she could use her ‘passion’ to understand why some people get allergies, and decided to become an allergy researcher.
Grant completed a Bachelor of Science (Medical Biotechnology) at Wollongong University and an Honors degree at the Garvan Institute/UNSW in Sydney, before moving to Melbourne where she completed her PhD at Monash University.
She now works at the Murdoch Children’s Research Institute in Melbourne, where she is an allergy researcher – a role she has held since July last year.
There, she suffered a terrifying incident of anaphylaxis during her lunch break last month.
A colleague sitting nearby was eating a salad that had satay dressing in it, even though some of it had probably splashed into her food.

Within moments, her throat became irritated and she began to feel faint and had difficulty breathing.
After realizing she was suffering from anaphylaxis – a potentially fatal allergic reaction – she alerted her colleagues, including the Institute’s allergy nurses, who took action.
Despite having had serious reactions before, it was the first time Grant had to use an EpiPen.
“It’s kind of scary to think you’re going to use this needle, which is quite big, but actually it wasn’t as painful as I expected,” she said.
She said the fact that she had been trained in how to administer it and that she “knew exactly what to do” helped her stay calm. But even with this quick action, she still required a trip to the emergency room for monitoring.

It was a sobering reminder of why she has dedicated her life not only to finding a cure, but also to supporting other allergy sufferers.
Since 2023, Grant has volunteered as a peer mentor with the National Allergy Council, a support-based organization that also operates Allergy 250K Camps.
The camps support the 250,000 children and young adults in Australia living with allergies.
The organization organizes separate camps every year for school-age children and young adults.
“We hold camps across Australia every year, which will be the first opportunity for some young children to spend a night away from home because they have such severe food allergies,” Grant said.
For a daily dose of 9honey, subscribe to our newsletter here.

“They also meet other children with severe food allergies, [where] Maybe they’ve never met anyone like them.
“[They can] also meet adults, people like me, so [they] hopefully can realize, ‘Yes, I have severe food allergies, but I can still go traveling, I can still get a good job.’
“It’s about sharing our experiences with young people.”
Attending the camps also reminds Grant why she is so focused on her work.
”I really want to understand what factors influence the development of allergies – why do we get allergies in the first place?” she said.

“And ultimately improve prevention strategies so that babies born today don’t have the same experiences, and that we can use evidence to guide therapies and prevention and also develop treatment options.”
Research obviously costs money.
The federal government recently announced $14.6 million in additional funding for the National Allergy Center of Excellence (NACE) and the National Allergy Council (NAC).
NACE, based at the Murdoch Children’s Research Institute, where Grant works, will use its share of the funding to accelerate its national allergy research, while NAC will continue to fund public health programs to support the 8.2 million Australians living with an allergic disease.
FOLLOW US HERE ON WHATSAPP: Stay updated with the latest celebrity news, lifestyle and opinions through our WhatsApp channel. No comments, no algorithm and no one can see your private data.